In the second installment of our five-part series, Healthcare AI and Infrastructure Dependency, we shift our focus from the power of individual AI innovations to the infrastructure that allows them to deliver lasting value. New AI technologies bring speed and capability, but in healthcare, the infrastructure, consisting of data platforms, workflows, governance, and trusted partnerships, creates a compounding advantage. Each successful deployment generates more data, stronger trust, and greater operational momentum, making the system more effective with every cycle.
Q: How should healthcare leaders think about the structure of healthcare AI within their organizations?
As healthcare organizations move from AI experimentation to real deployment, a new question is emerging: How should AI actually be structured within the enterprise? Efforts often begin as isolated pilots, individual tools embedded in departments or introduced through specific vendors. As AI becomes more embedded in clinical, operational, and administrative workflows, organizations are realizing that a more deliberate structure is needed. Questions around governance, data ownership, platform strategy, and clinical oversight are becoming just as important as the technology itself. ^1 The challenge for healthcare leaders is to determine where AI capabilities should live within the organization and how to design a structure that allows innovation to scale while maintaining alignment, accountability, and patient safety. ^2
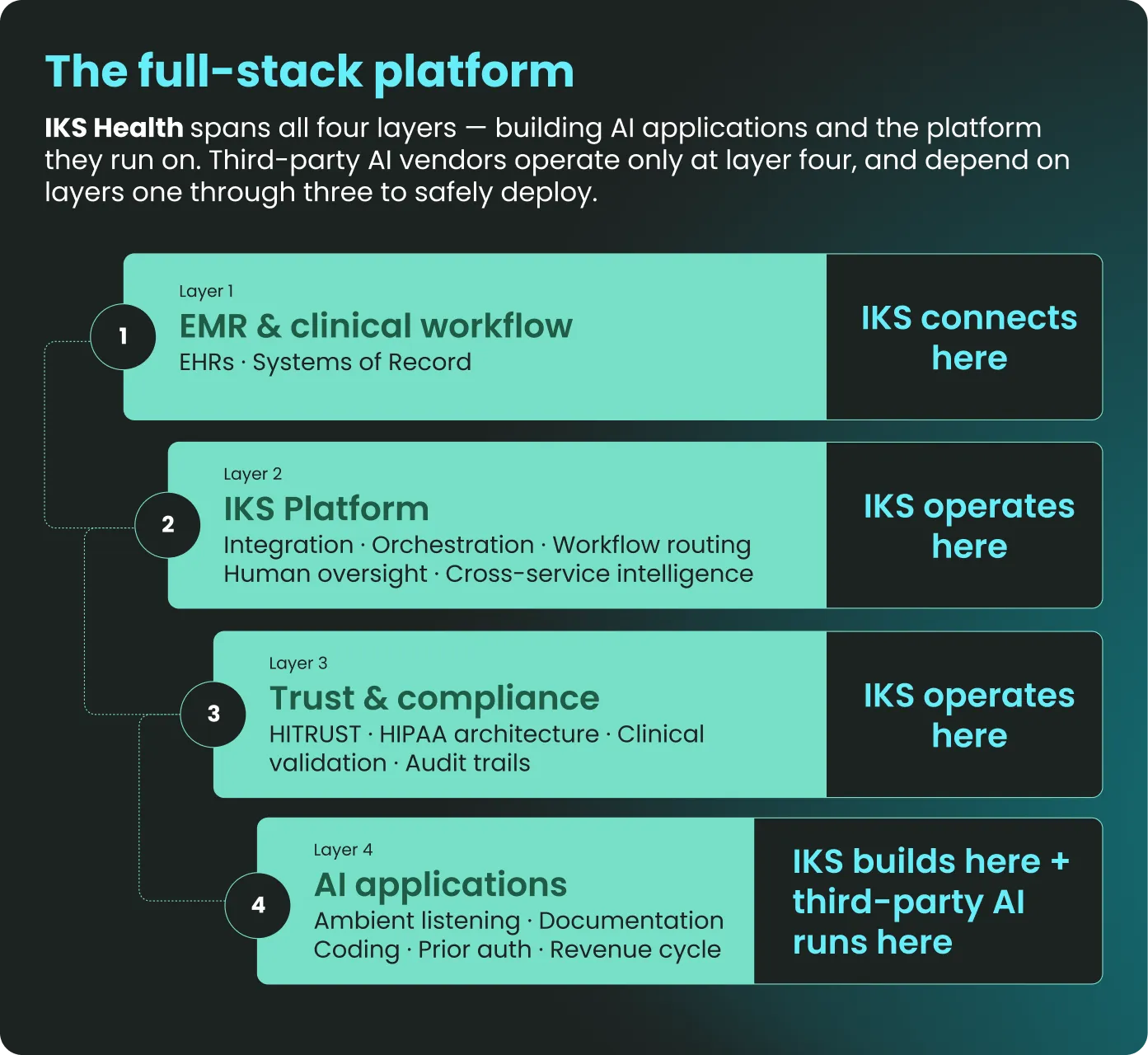
At IKS Health, we believe healthcare AI can be organized as a full four-layer stack, where each layer works together safely and efficiently. Industry research supports this ‘operating system’ approach, noting that 70% of AI success is driven by workflow and orchestration rather than the AI model itself. ^3
Layer 1: The EMR and clinical workflow. These systems of record are where patient data lives, and clinical work happens. Every AI application must ultimately read from and write back to this layer.
Layer 2: The integration and orchestration platform. This is where IKS Health’s care enablement platform operates, sitting between the EMR and the AI applications, to manage data flow, workflow routing, and cross-service intelligence while providing human-in-the-loop oversight. We are the connective tissue, creating a trust infrastructure.
Layer 3: The security and compliance infrastructure. This layer encompasses HITRUST certification, HIPAA-compliant architecture, clinical validation protocols, and audit trails. Governance and data sovereignty have become the primary prerequisites for enterprise AI.^4 These are not merely features; they are prerequisites that live on the IKS Health platform rather than within any individual AI model.
Layer 4: The AI applications. These consist of ambient listening, clinical documentation, medical coding, prior authorization, and revenue cycle optimization. Whether these capabilities are built by operating system infrastructure companies like IKS Health, foundation model companies, or specialized vendors, safely deploying AI in healthcare requires comprehensive integration with systems of record, robust security and compliance, and human-in-the-loop oversight across the full connected care journey.
Consider what happens when a health system tries to adopt AI applications without an operating system. They may buy an ambient listening tool independently from a coding tool, separate from a prior authorization bot, and a revenue cycle optimizer. This can create four separate integrations with the EMR, four separate compliance reviews, four separate data silos, and four separate vendor contracts, with zero cross-service intelligence. Market analysis suggests that this ‘point solution fatigue’ is driving a massive industry shift toward platform consolidation.^5
IKS Health is uniquely positioned as a fully integrated care enablement platform leveraging AI to bring all of these disparate capabilities together seamlessly. Our integration ensures the ambient listening tool knows what the coding AI found, the coding AI knows which prior authorization was denied, and everything is tied to the revenue cycle tool. This cohesion is essential to maintaining the margins to care that allow clinicians to focus on patients rather than process.
Q: Explain the compounding effect. How every clinical encounter makes AI smarter and more valuable.
In a healthcare environment, every encounter that flows through a platform generates signals that improve every service, creating a compounding effect. The system becomes more valuable the more it is used, leveraging patient care, clinical workflows, and operational data to generate greater insight and efficiency over time. As data accumulates and AI tools learn from real-world care delivery, the platform becomes increasingly effective and significantly harder for competitors to replicate or displace.
More specifically, the ‘data network loop’ is what drives this compounding value. Every clinical encounter generates training data, which improves model accuracy. In turn, each accuracy gain reduces the need for human review, lowering costs and improving margins. This efficiency enables more clinical encounters, creating a repeating cycle that strengthens the system with every iteration over time.
Unlike new entrants that start with zero encounters, an integrated care enablement platform like IKS Health begins with the advantage of millions of cumulative encounters. This ‘data network loop’ is now recognized by healthcare investors as the primary driver of long-term value, as cumulative data encounters create a barrier to entry that standalone AI startups cannot match.^6
IKS Health integrates into the EMR, the clinical workflow, the billing system, and the payer submission process. Replacing a single AI tool with another often requires rewiring the entire clinical-to-financial data pipeline, creating significant customer switching costs. Furthermore, assets such as HITRUST certification, clinical validation track records, and established customer references reflect years of accumulated trust that cannot be fast-tracked.
IKS Health has earned this trust over twenty years of clinical operations. Our deeper, more integrated platform allows our coding models to improve with every documented encounter. Our prior authorization predictions sharpen with every denial pattern, and our revenue cycle optimization is refined with every resolved claim. This is a compounding advantage with patterns learned that improve outcomes for every health system on the platform.
Q: How does the compounding advantage apply in a real-world patient encounter?
Let’s walk through an IKS Health intelligence chain and trace one patient encounter through our highly integrated platform.
Clinical Documentation: The ambient listening tool captures the physician-patient interaction and generates structured clinical notes. Rather than simply storing them, it flags coding-relevant clinical indicators and pushes them downstream.
Medical Coding: The IKS coding engine receives these indicators alongside the full documentation. It assigns diagnosis and procedure codes while identifying potential under-coding, specificity gaps, and documentation deficiencies, routing them back upstream for physician review before submission.
Prior Authorization: When codes trigger payer requirements, our prior authorization system already possesses the clinical documentation, the coded encounter, and the patient history. It generates authorization requests with supporting evidence pre-attached, reducing denials and turnaround times.
Revenue Cycle Management: The billing and collections process inherits the entire chain: the documentation, the coding rationale, and the authorization status. When a claim is denied, our system traces the reason back to the specific clinical documentation gap and flags it for the next encounter. No point solution can achieve this, not because the AI isn’t ‘smart’ enough, but because it lacks access to the full chain and twenty years of accumulated clinical intelligence. By streamlining this connected care journey, IKS Health restores the margins to care necessary for sustainable healthcare delivery.
This ‘agentic AI’ approach, where AI agents communicate across the full care journey, was recognized as a gold standard for 2026, helping health systems restore the margins to care.^7
Sources:
^1. ^4. 2025 Watch List: Artificial Intelligence in healthcare (NCBI / CADTH)
^2. Healthcare doesn’t need more point solutions (Notable Health)
^5. AI in Healthcare: Why VCs are doubling down on platforms (TechEquity AI)
^6. IKS Health debuts agentic AI platform at AMGA (IKS Health)
^7. Top honors in AI-driven RCM and coding (Black Book Research)